FUNGAL INFECTION (ONCHOMYCOSIS)
ONYCHOMYCOSIS
What is it?
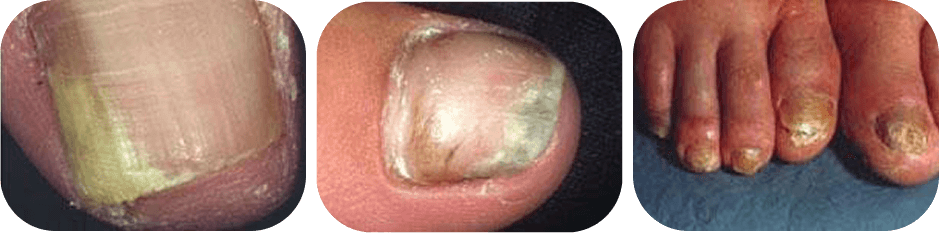
Onychomycosis is a fungal infection that affects one or more toenails and/or fingernails, most commonly the great toenail or the little toenail. It presents in various patterns, often seen as whitish to yellow-brown discolouration or nail splitting. In some cases, it may be associated with pain in the nail folds.
Who gets it?
Onychomycosis is commonly found in adults. It can occur due to weakened immune system, poor circulation, or trauma to the nail. Fungal infections are often seen in individuals who wear tight-fitting shoes or those with moist, tropical environments that promote fungal growth.
Causes
- Fungal Exposure: A common cause is contact with fungi in damp environments such as locker rooms, communal showers, and swimming pools.
- Trauma: Injury to the nail can create an entry point for fungi.
- Underlying Conditions: Diabetes, poor circulation, and immunocompromised state can increases the likelihood of developing onychomycosis.
Symptoms
- Discolouration of nails (whitish, yellow-brown).
- Nail thickening, splitting, or crumbling.
- Pain or sensitivity around the nail folds.
- Infected nails may detach from the nail bed in severe cases.
Diagnosis
- Nail Clippings: Samples can be taken from crumbling or discoloured tissue at the end of the affected nail.
- Debris Collection: Scraping the nail surface or collecting debris from beneath the nail can help identify fungal elements.
- Dermatoscopy: A non-invasive technique used to visually examine the nail for specific patterns suggestive of fungal infection.
- Nail Biopsy: In some cases, a biopsy may be done to detect histopathological signs of onychomycosis.
Treatment
- Mild Infections: For less than 50% involvement, topical antifungal medications may be sufficient.
- Moderate Infections: Oral antifungal medications are required for several months.
- Severe Infections: In cases where the infection is extensive or resistant to medication, a combination of oral and topical treatments is often recommended. In some instances, surgical nail removal may be necessary to fully eliminate the infection and encourage healthy regrowth.
Non-Drug Treatment
- Recent advancements in treatment have introduced non-drug solutions like laser therapy to treat onychomycosis, avoiding the side effects of oral antifungals.
- Devices Used for Treatment:
Nd:YAG continuous, long or short-pulsed lasers for effective fungal treatment.
PARONYCHIA
What is it?
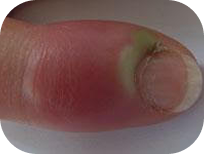
Paronychia is inflammation of the skin around the fingernail or toenail. It can be either acute (lasting less than 6 weeks) or chronic (persisting longer than 6 weeks). It’s often seen following a break in the skin, such as from nail biting or ingrown toenails.
Causes
- Acute Paronychia: Most commonly caused by bacterial infections (e.g., Staphylococcus aureus), but can also be caused by viruses (Herpes simplex).
- Chronic Paronychia: Often linked to dermatitis around the nail fold, usually affecting people who frequently have their hands in water or are exposed to irritants (e.g., dairy farmers, housekeepers).
What do you see?
- Acute Paronychia: Rapid onset of pain, redness, swelling, and sometimes pus-filled lesions. Fever may accompany more severe cases.
- Chronic Paronychia: A gradual process that may affect multiple nails over time. The affected nail folds may become swollen and lifted off the nail, with occasional pus discharge.
Diagnosis
Paronychia is primarily diagnosed through clinical observation, with additional lab tests confirming infection:
- Gram Stain Microscopy: To identify bacteria.
- Potassium Hydroxide (KOH) Test: For fungal identification.
- Pus Culture and Sensitivity: Helps identify the specific pathogen and determine the most effective antibiotic treatment.
- Viral Swabs and Tzanck Smears for viral infection.
- Nail Clippings for mycology culture.
Treatment
Acute Paronychia:
- Place the affected finger or toe in warm water for 15–20 minutes, several times a day, to reduce swelling and promote drainage.
- Topical antiseptics can help prevent the spread of infection.
- Topical antibiotics (for bacterial infections) or antifungal creams (if a fungal cause is suspected) may be prescribed.
- Oral antibiotics, antivirals, or antifungal medications may be necessary for more persistent or widespread infections.
- Anti-inflammatory drugs (e.g., ibuprofen) may be used to relieve pain and reduce inflammation.
- Surgical incision and drainage may be required if an abscess has formed.
- In severe or non-healing cases, partial nail removal might be performed to allow proper drainage and healing.
Chronic Paronychia:
- Preventive Care: Keep hands dry and avoid prolonged exposure to moisture.
- Topical Treatments: Apply emollient hand creams to reduce inflammation.
- Antifungal Agents: Oral or topical antifungal treatments may be necessary in resistant cases.
Prevention Tips
- For Acute Paronychia: Avoid biting nails or picking at the cuticles, and protect your nails from injury.
- For Chronic Paronychia: Ensure hands remain dry and clean, especially if you work in moist environments. Consider wearing waterproof gloves when handling water or harsh chemicals.

